Over 100 Irish women travelling to Romania for endometriosis surgery every year
A Romanian surgeon has said that some Irish patients who visit his clinic had surgeries using methods that made their next one ‘more difficult’.

BETWEEN 100 AND 150 Irish women a year are travelling to Romania for surgery for endometriosis, as the Irish health service struggles to find the resources to treat the chronic disease.
A senior person at Ireland’s only endometriosis charity has said there is a narrative forming among women with endometriosis that it is ‘better to go abroad in the first instance for treatment’.
The HSE has acknowledged that treatment for endometriosis has been ‘under-resourced and under-funded’.
Endometriosis, often referred to as ‘endo’, is a chronic disease that sees tissue similar – but not the same as – the lining of the uterus grow in other places. It’s usually found in the pelvic region, but can be found anywhere in the body.
Endo is not a menstrual condition, but it’s often triggered in girls when they begin to get periods, and it can cause intense pain that is debilitating in some cases and heavy bleeding during periods.
Endo can also cause infertility, and for some women who don’t experience painful symptoms, it can be discovered later in life when they are trying to conceive.
Health Minister Stephen Donnelly announced the development of a new national framework for endometriosis last year, which will see GPs, five regional endo hubs, and two supraregional centres in Dublin and Cork forming a defined clinical pathway.
Recruitment for new posts in these centres is ongoing. It’s understood that some of the agreed posts haven’t been recruited for or filled as a result of the HSE’s recruitment freeze, such as the clinical psychologist post in the Tallaght clinic.
In the meantime, women are still travelling abroad for surgery, some of whom have had several surgeries in Ireland that they feel left them in a worse state in the long run.
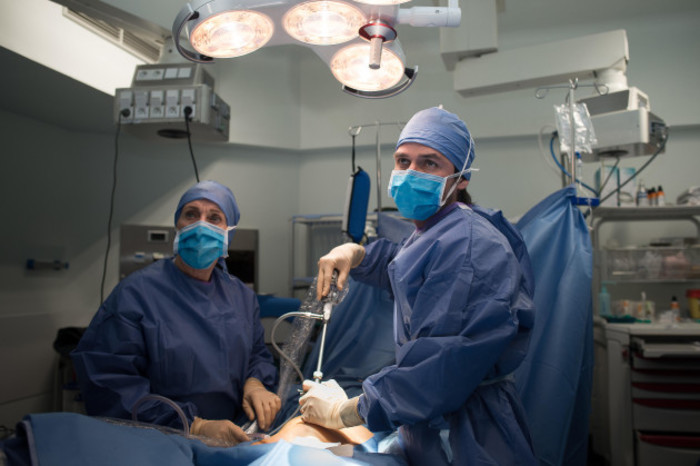 Picture of endometriosis examination taking place in a European clinic.
Picture of endometriosis examination taking place in a European clinic.
Noteworthy, the crowdfunded community-led investigative platform from The Journal, supports independent and impactful public interest journalism.
‘Unnecessary trauma’ on patients
There is a lack of research in this area, but experts generally agree that in most cases a process known as excision is the best surgical method for removing endometriosis lesions, rather than the other option of ablation.
Dr Gabriel Mitroi, the co-founder of the Bucharest Endometriosis Centre, told The Journal that excision removes endometriosis tissue “from its roots”, while ablation “burns away” tissue on the surface, rather than fully removing it.
His clinic only uses ablation in cases where endometriosis is on the ovaries, and the patient wants to preserve their fertility.
He said that some Irish patients that come to his clinic who’ve had surgeries in Ireland have formed “adhesions” in their pelvic region as a result of ablation being used.
“It is only postponing the pain, and it is an unnecessary trauma on the patient,” he said.
“This makes the next surgery more difficult,” Dr Mitroi explained, adding that previous surgeries may result in the removal of organs when it is “not necessary”.
Overall, Dr Mitroi said that it is not his place to “criticise” the standard of endometriosis care in Ireland. “I am sure they are doing the best they can with the information they have. I too wasn’t able to operate or diagnose the disease in the beginning, it takes a lot of effort, and you need to be self-taught, as there is no training available,” he added.
Damien Donoghue, vice chair of the Endometriosis Association of Ireland, told The Journal that there is a lack of excision specialist surgeons in Ireland, and that the guidelines for endo care than the HSE are soon to publish “do not go far enough”, but that they offer “a starting point”.
Donoghue said that the lack of experienced surgeons in this field has lead to some women, including his ex-partner, having or being offered surgeries that involve a bowel or bladder resection (where part of the organ is removed) as part of their surgery, when an excision specialist could have potentially removed the endo tissue, but saved all of the organ.
He was critical of some of the work done by some surgeons. “But we also have a handful of specialist surgeons in Ireland who are experienced in this field and are at the forefront of improving endo care,” he said.
Damian adds that some of the HSE “hubs” consist of two healthcare professionals. He explained:
A clinical nurse specialist and a physiotherapist does not make a specialist centre, and that is not the standard you’d see in endo centres abroad.
Donoghue believes that we are at an important crossroads when it comes to the future of endo care in Ireland.
“There is a narrative forming, which is partly informed by people who are speaking from their own experiences on social media, that it is better to go abroad in the first instance for treatment. That’s not necessarily the best course.
“There can be complications after surgery, and though a lot of centres offer a high standard of care, they are offering a for-profit service, and that needs to be considered,” he said.
 Damien Donoghue, vice chair of the Endometriosis Association of Ireland, speaking at the Oireachtas Health Committee last year.
Damien Donoghue, vice chair of the Endometriosis Association of Ireland, speaking at the Oireachtas Health Committee last year.
Years of women suffering
Dr Alison DeMaio is a gynaecologist at Tallaght University Hospital’s endometriosis service.
At the Endometriosis Association of Ireland’s (EAI) annual conference last weekend, she said that the announcement of the endo national framework last year came after years of women suffering due to treatment delays, needing to go to the emergency department for pain flare ups, and “not having their voices heard”.
In the last year, things have gotten “a little brighter” for those trying to get a diagnosis, and those with endometriosis who need treatment.
DeMaio said that her team is “evolving rapidly”, and that both she and Dr Aoife O’Neill now have dedicated theatre time for endo patients, and the clinic sees patients once a week, rather than once a month.
“We are seeing up to 60 patients each month, and we’d like to get 80. Instead of assessing 220 women per year, we’d be seeing over 900,” she said.
Many girls and women with endo go down a long road of referrals before they get to see a specialist team like the one at Tallaght, as they are often referred to a general gynaecologist by their GP.
A 17-year-old with suspected endometriosis who attended the conference asked DeMaio if there are any specialists who could see her.
“I’ve been seeing gynaecologists as I have suspected endometriosis, but the doctors I see are confused…
During my period it is very debilitating, and the inflammation on my hips is so bad that I need to use a wheelchair for that week in school.
I’m being bullied by other students, because I’m in a wheelchair some weeks, but not others. They are making fun of me. If you know any doctor who could help me, I’d be very grateful,” she said.
Many of the nearly 200 women in the room, most of whom have lived with endo for years, were shaking their heads while listening.
Dr DeMaio said: “I’m really, really sorry. I actually feel quite emotional. If you were referred to a service like the one we have in Tallaght, there is a lot we could do for you.”
There is a six month waiting list for an initial assessment with the Tallaght clinic.
Donoghue, from the EAI, said that it is “amazing” to have a highly specialised service in the country being expanded, but that it cannot cater to the thousands of women who are being impacted by this condition.
“We need to get behind Dr DeMaio and the gynaecologists like her who are changing the way that endometriosis is treated in Ireland, so treatment abroad isn’t the only option for women with complex endo in the future.
“The endo community also needs to join together to get our message across to politicians. There’s still too much squirming about this, because it’s a women’s health problem.
“If endometriosis isn’t one of the health issues on their radar come the next election, progress will stall, and these women will be forgotten about for another five years. That can’t happen,” he said.
Senator Lisa Chambers, who also attended the conference with her sister (who has been diagnosed with endo) said: “One of the big challenges is that, for endometriosis surgery, particularly in complex cases, it takes a multi-disciplinary team, if you are operating on the uterus, the ovaries, the bowel, it’s not simple and you are in theatre for quite some time. But those cases are in competition for theatre time and because they aren’t classed as emergency life-saving surgeries, they will often come last”.
Chambers added that it is important that people diagnosed with endo know that “it isn’t all doomsday”, and that there are gynaecologists in Ireland that can treat and help them.
As of February of this year, over 34,000 women and 600 children were on the waiting list for gynaecology appointments or procedures.
That’s over 200 more women compared to February 2023. Over 800 of these women have been waiting for over 18 months, which has gone down from almost 2,000 women in the previous year.
This data isn’t endometriosis specific. Records released under the Freedom of Information (FOI) Act show that gynaecology was one of the top types of inpatient care the HSE funded patients travelling abroad for in 2023, under both the EU Cross Border Healthcare Directive and the Northern Ireland planned Healthcare Scheme.
The schemes cost the state €9,002,407 and €15, 684,435 last year respectively, for a wide range of treatments. While gynaecology wait lists don’t capture how many women are waiting on procedures for endometriosis, they also don’t capture how many have given up on pursuing surgical solutions in Ireland.
The Bucharest Endometriosis Centre isn’t the only specialist clinic in Europe, and Irish women also travel to the UK for surgery and treatment. The number of women who travel abroad for endo surgery each year is not known.
—
Read more articles in this series >>

Are we taking women’s health seriously in Ireland?

By Eimer McAuley for The Journal and Noteworthy
This investigation was done as collaboration between The Journal and Noteworthy. It was part-funded by you, our readers, with support from The Journal as well as the Noteworthy investigative fund to cover additional costs.
What’s next? We want to examine why waiting lists for life-saving scans are so long? Help fund this work >>






