Female junior doctors repeatedly penalised by medical training system
Women make up more than half the trainee doctor workforce but criticise lack of support for pregnancy and family life.

“RIGHT NOW, I would not recommend that a woman go into my field.”
Kate* is a trainee hospital doctor. Until recently, she never felt disadvantaged as a woman in her field and that “hard work was rewarded”. Until, that is, she started planning a family and was hit by problems that her male colleagues do not face.
Now she says that with hindsight she wouldn’t have taken this path.
She found out that she would be forced to move to another part of Ireland with her six-month-old as soon as she finished maternity leave, and that because of where she was in her training, she was ineligible for maternity pay.
As a result, she took a big financial hit, and had to extend her training by a year.
This is at a time that the HSE is working hard to attract and retain doctors.
Kate is one of the many female non-consultant hospital doctors (NCHDs), also known as junior doctors, who spoke to Noteworthy for our SPECIALIST CARE investigation.
They had already faced extremely tough conditions working in Irish healthcare for years but never felt so unsupported as when they started planning families. A number delayed or dropped out of training schemes or reconsidered their choice of career altogether – or are advising younger staff to do so.
The Irish healthcare system relies on NCHDs but they are particularly vulnerable because they work on short, insecure contracts, for long hours and must move around the country regularly throughout their training with little advance notice.
This particularly affects women. More than half of NCHDs are female.
One junior doctor quoted in the recently published government NCHD Workforce Report said that many women “would like to continue working in the hospital” but this becomes infeasible for many “due to rotation locations and inability to get out on time (before 7pm)”.

Noteworthy, the crowdfunded community-led investigative platform from The Journal, supports independent and impactful public interest journalism.
Noteworthy put the issues raised by women, including short notice for geographical rotation, lack of support during pregnancy, problems with maternity pay and the unavailability of childcare, to the HSE.
A HSE spokesperson said that they had a number of policies in place to help doctors with pregnancy as well as to balance work and family life.
They said that significant work had been done in recent years to make training scheme rotations more predictable and welcomed the recommendations made in the NCHD report, published in February.
All the women we spoke to work in medical and surgical disciplines and are, or were, on track to become consultants. The Royal College of Surgeons Ireland (RCSI) and the Royal College of Physicians of Ireland (RCPI) oversee the training of the doctors we interviewed but there are other training bodies in operation.
The RCSI told Noteworthy that “promoting gender balance in surgery is a key strategic objective”. A spokesperson said: “We have had a particular focus on women in surgery for a number of years.”
Noteworthy also put questions to RCPI and the Forum of Irish Postgraduate Medical Training Bodies (The Forum) – an umbrella organisation for the training bodies. Neither responded in time for publication.
Fear that women will drop out of medicine
The Irish Medical Organisation (IMO) has warned that gender inequality is significant in medicine in Ireland and contributing to staffing problems.
“At a time when our health system is chronically understaffed, we need to be doing everything we can to both recruit doctors and retain those already working in the system,” said Dr Madeleine Ní Dhálaigh at an IMO conference last year.
“We know from an IMO survey that female doctors compare poorly to their male counterparts when it comes to issues including childcare, gender discrimination and gender-based harassment.”
The Chairperson of NCHD Committee at the IMO, Dr Rachel McNamara, told Noteworthy: “Without support women will drop out of medicine.”
The government NCHD report, published in February, aims to improve conditions for NCHDs through a number of measures, including reducing the numbers of moves they must make, giving them more warning of moves and providing childcare at hospitals.
Female NCHDs told Noteworthy that these measures can’t come quickly enough.
“Overall, it’s definitely a much better environment for women than it was before,” said Kate, who added that it’s not where it needs to be. “There’s still real challenges.”
Data shows, for example, that under the age of 44, there are more female consultants than male, although there are more male consultants overall.
There is also a large drop off as surgical trainees progress through the ranks.
When this was put to the RCSI, a spokesperson told Noteworthy that it has increased the proportion of women surgical trainees to around 45-50% across training levels and all specialties. It also launched a Women in Surgery Fellowship to support female surgeons, according to the spokesperson. The Fellowship supports one woman a year.
The HSE did not respond directly when asked about retention rates and what it is doing to retain female NCHDs, given that the latest HSE retention report does not mention gender.
A spokesperson directed our team to the annual medical workforce reports. Noteworthy used gender data from these for our graphs which demonstrate the stark dropoff of female doctors at higher levels in hospitals.
Hospitalised because of stress
Kate told Noteworthy that she delayed starting a family until later in her career because she hoped that, as a more senior doctor she’d have more choice about where she could work.
She requested to stay in the area where she and her husband own a house and have family support, including childcare, as “you have to arrange these things so far in advance”.
However, while pregnant, she was told that she would be posted to a hospital in a different city as soon as she came back from maternity leave. “This is despite me saying it would cause significant difficulties” from a financial and family perspective, she said.
“I ended up in [hospital] with complications as a result of the stress.” Because of this, she said: “I just accepted the post rather than fighting it. Because I felt like I couldn’t for my health.”
Experiences like Kate’s are not unusual, according to IMO’s McNamara. Although there are moves to change this, you could get as little as a couple of months’ notice of where you’re going next. She added:
Long-distance marriage is very common.
Kate has delayed resuming her training scheme until her child is two or three. “I still have to go [to another city], it’s still going to be a huge issue,” she said. “But at least I have time to plan it.”
The HSE told Noteworthy that “this is an area that is kept under constant review” and that it welcomes the recommendations on reducing geographical moves in the recent NCHD report.
The spokesperson said that trainees receive “a minimum of two years pre-defined rotations” and that they get this “a minimum of 13 weeks” prior to starting their training scheme and also before their third year of the scheme.
In 2017, RCSI committed to allocate training posts more than 12 months in advance, something which one female surgical trainee told us “categorically does not happen”.
When we put this to RCSI, a spokesperson said that “giving notice of rotations of 12 months is not feasible” in the first two years of training because of the short timeframes and qualification requirements.
“However, we do work directly with individual trainees to minimise geographical disruption when balanced with their choice of specialty,” they added.
For the following six years of higher specialist training, the spokesperson said that “RCSI gives a minimum of two years notice on such rotations, and longer where possible”.
Not all the women Noteworthy spoke to got this much notice.
RCSI committed to reporting annually on how often they give 12 months’ notice to trainees, broken down by gender. When Noteworthy asked for this data, RCSI did not provide it.
The RCPI and the Forum did not respond in time for publication.
Unpaid maternity leave
Because Kate became pregnant while taking time off her scheme to do research as part of her training, she discovered that she was not eligible for maternity pay.
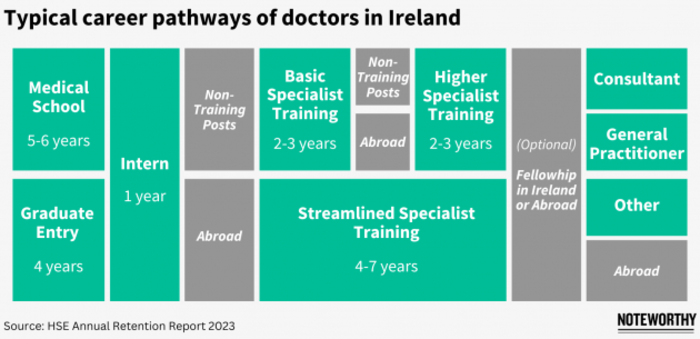
NCHDs like Kate are on a training scheme and are called ‘specialist trainees’. They are managed by training bodies and are on a direct track to becoming consultants. Those who are not on a scheme are non-training NCHDs and manage their own career progression. These doctors make up almost 40% of all NCHDs.
Ireland has one of the lowest ratios of consultants to population.
“We don’t need more [non-training] NCHDs, we need to convert them to consultants,” said Dr Seán Casey, one of two national lead NCHD fellows at the HSE who was also involved in producing the NCHD recommendations.
“The quickest way to get a consultant is to put someone on a training scheme.”
Coming ‘off scheme’ to do research as part of a doctorate programme is a common pathway for specialist trainees and is counted as a year of their qualification towards becoming consultants.
Women on training schemes told Noteworthy that although research isn’t obligatory, it is expected in order to be competitive in some areas of medicine. But depending on the location of research – for example at a university or a private hospital – women may not have access to paid maternity leave.
“It’s absolutely outrageous,” said Casey, when asked about cases like Kate’s, “especially when there’s an onus on people to do [research]”.
Noteworthy asked whether the HSE finds it acceptable that women who go off-scheme to do research as part of their training aren’t necessarily entitled to paid maternity leave.
A spokesperson said that “all NCHDs employed by the HSE are entitled to full maternity leave benefits” but didn’t comment on those undertaking research.
On this, the RCSI responded that “the issue relating to paid maternity leave is a matter for the HSE as the employer”. The spokesperson said: “We understand that NCHDs in the HSE and HSE-funded hospitals are entitled to the same level of maternity support as all employees in the HSE.”
We put the same question to the Forum and the RCPI but they did not respond in time for publication.
Ciara* is a specialist trainee in internal medicine currently doing research. She would like to start a family but told our team that she is not entitled to paid maternity leave.
“If you’re looking at gender-specific problems, this inevitably affects females,” she said.
It’s very difficult for anyone to have a baby without access to maternity [leave].
It “really stings, because I’ve worked so dreadfully hard over the last few years, and I see all my friends around me having no worries about [having children],” she said.
Ciara paid around €60,000 to complete a graduate entry medicine course so isn’t in a position to try for a baby with her partner until she’s eligible for paid maternity leave, at which point she’ll be in her late 30s.
She is anxious about a decline in her fertility and this impacting her ability to have children.
“Five years ago I would have said ‘no way that would come first, I’ll just have a baby and I’m never going to allow my job to interfere’ but you just can’t help that happening, unfortunately, once you’re in it.”
Ciara has moved eight times in ten years for her training. You “can’t go to a random house share” with a new baby, she said, and her partner didn’t want to be, effectively, a single father if she was rotated away from home.
As well as some NCHDs not getting paid for maternity leave, there are also issues for women in taking it as well as finding a job after it, said IMO’s MacNamara.
NCHD lead Casey confirms this. “The system is designed so that all doctors start a contract in July and come off it in July or January.”
When people come back from maternity leave, “it gets messy”, he said. “The system struggles to support that.”
 Health Minister Stephen Donnelly launches the NCAD workforce report in February 2024.
Health Minister Stephen Donnelly launches the NCAD workforce report in February 2024.
Impact of work conditions on pregnant doctors
Concerns over hospital working conditions during pregnancy were raised by all the women that Noteworthy spoke to.
Many pointed our team to 2019 research which found that surgical trainees in Ireland were much more likely to have problems during pregnancy than either their female non-surgical colleagues or partners of male surgical and non-surgical trainees.
Their concerns echo an IMO survey in 2017 which found that, of the respondents who had been pregnant, “84% stated that no member of staff discussed their pregnancies with them to ascertain whether health risks arising from the performance of their workplace duties existed”.
Female trainees told us that the decision about when they should stop being on the on-call rota while pregnant came down to the understanding of their team. Those who had a positive experience repeatedly used the word “luck”.
“I just got really lucky,” said one NCHD. It was “definitely not a reflection of the majority” and “depended on help from supportive colleagues rather than systematic support”.
NCHD Clare O’Connell has a two-year-old daughter and is pregnant with her second child.
“I think the training schemes were originally designed with the kind of archetypal male doctor in mind, whose partner could follow them around the country, and maybe wasn’t working,” she said. “And now the way it’s set up doesn’t suit men or women.”
O’Connell is a specialist surgical trainee in urology. She is satisfied with her training and would pick urology again. However, she also said her career has been one of “meticulous planning and good luck” in terms of where she’s been placed.
She also said that it was difficult being pregnant and doing the work – particularly being on the on-call rota.
She said she probably stayed on this rota too long into her pregnancy but there’s a culture of keeping working. “There’s very little wiggle room built into the system,” she explained. If one person from the team is missing, colleagues “are left scrambling to cover and that’s what the whole system is based on”.
I’m only able to [do this work] because my husband has a career that allows him to do 70 – 80% of the childcare.
In the latest Irish Medical Council report, almost 30% of doctors worked more than 48 hours per week. Among trainee specialists, this rose to 50%.
“The job leaves very little space for anything else,” said Dr Niamh Humphries, head of research in the Graduate School of Healthcare Management at RCSI.
Noteworthy asked the HSE whether it has guidelines on when pregnant women should stop on-call work. A spokesperson said that the HSE is subject to laws that govern safety at work and that they have issued additional, specific guidance on pregnant employees at the HSE. They added:
“If necessary, action must be taken to ensure that the employee is not exposed to anything that could damage either their health or that of their developing child.
“Managers must assess the factors in work that can impact any aspect of pregnancy, including tiredness, overtime, evening and night and shift work.”
Long hours and childcare issues
According to the IMO, almost half (46.5%) of female doctors with children said they were “mainly or fully responsible for childcare within their family” compared to 6% of male doctors. It also found that 92% of women had taken some kind of leave to care for children or relatives, compared to 30% of men.
“Mothers are struggling,” said Audrey*, a single mother and senior NCHD working in a child health role who told Noteworthy that she’d already taken all the annual leave allocated for this year to care for her child.
“You’re praying for a solution, you’re struggling and you can’t cope.”
A 2021 study, led by RCPI, found that female doctors in Ireland felt unable to speak up for themselves at work. Many were “particularly concerned about acquiring reputations that played into gender stereotypes”.
Audrey felt that there’s a high lack of understanding of what it is to be pregnant or a mother and a NCHD. “We don’t talk about it at work,” she said.
She dropped out of the specialist training programme to work as a non-training NCHD, thereby taking a pay cut, because she says she “couldn’t keep it up”.
The HSE told Noteworthy that it had a number of policies in place to support work-life balance, including flexible working and job sharing.
“There is no specific policy in respect of the provision of childcare facilities on-site,” said the spokesperson. “However the feasibility of individual sites providing these facilities is something that can be considered by services locally.”
 A NCHD protest over ten years ago against dangerous working hours in Irish hospitals.
A NCHD protest over ten years ago against dangerous working hours in Irish hospitals.
Cost of solutions minimal
Some positive changes have already been made. In 2022, the Irish Medical Council made it possible for women on maternity leave to claim back 50% of their annual registration fees. Before that, women were paying full price to remain on the medical register, even when they weren’t working.
“The message it sends is powerful,” said NCHD lead Casey.
He added that the need for further change is “becoming more and more important” because there are more female doctors and “we’re seeing an ageing medical workforce”.
Many of the recommendations in the NCHD report, such as making work more predictable, are due to be implemented in 2024.
Noteworthy asked the HSE for details for the implementation, especially given a current HSE hiring freeze. A spokesperson responded that the report “is being considered in the context of the Pay and Numbers Strategy 2024 which will shortly be agreed with the Department of Health”.
If implemented, geographical moves would be better coordinated and more warning given. There would also be better support for mothers returning to work.
Many, like Kate, made the point that some of the most impactful measures are about planning, rather than investment.
RCSI’s Dr Niamh Humphries welcomed the report’s recommendations but said:
“Implementation is key – there is a lot of good research sitting on shelves not informing practice. That disconnect needs to be bridged to leave impact on the ground.”
*Names have been changed

Are we looking after our specialist trainees?

By Alice Chambers of Noteworthy
Noteworthy is the crowdfunded investigative journalism platform from The Journal. This project was proposed and funded by our readers alongside significant support from our investigative fund.
What’s next? We want to examine why waiting lists for life-saving scans are so long. Help us investigate >>