'Unheard, belittled and made feel small': Women still battling for maternity care choice
Noteworthy’s months-long investigation reveals inconsistent care and lack of choice leading to trauma and unnecessary medical interventions.

“IF YOU DON’T know that you have a choice, then you don’t have a choice,” Orla Harrington, mother of two from Co Louth told Noteworthy.
Though she wanted a home birth for her first pregnancy, she found “roadblocks everywhere” she turned.
Obstacles are stopping women from choosing the maternity care they would prefer, with those in rural Ireland facing even more limitations.
Our months-long investigation reveals inconsistent care across Ireland, frustrating women who are treated differently due to local policies that impact how medicalised their birth will be.
We show how a key care choice – alongside birthing centres – promised under the National Maternity Strategy is being delivered by the HSE in a diminished form. Just two of these units are in place – the same number as before the strategy was developed.
Pregnant women are being discharged by GPs as one of the main insurance providers in Ireland does not cover home births. Little action has been taken to address this by either the Department of Health or the HSE.
Lack of choice is not only causing trauma and unnecessary medical interventions, but also costing some thousands. Some private home birth packages can set expectant mothers back over €9,000.
As part of our BIRTH PLACE investigation – being published across this week – over 20 women from all over Ireland who gave birth within the past two years spoke to us about their pregnancy and birth experiences. Our team focused on women who want choices beyond hospital care to assess available options.
Despite some reform, we find women are still fighting to be heard at every stage of their pregnancy, with many feeling that they are not in control of their care.
FIRST TRIMESTER: You’re pregnant, what now?

Once two lines appear on a pregnancy test, the first port of call for most is a GP.
When Harrington went to hers, understandably, she had lots of questions. She asked about home birth but “was strongly advised against it and given zero information about it”. Feeling very discouraged, she opted for hospital care.
Almost all – over 85% – women Noteworthy spoke to told us that their GP asked them just two questions: What hospital do you want to go to? Public or private?
No other choices, or the implications of these options, were discussed.
Harrington “immersed” herself in research following the birth of her son and booked a home birth midwife before going near her GP for her second pregnancy.
“I just knew from hearing other people’s stories… It wasn’t something that was divulged freely.”
Orla on pushback from her GP: ‘There were roadblocks everywhere’
GPs may feel that it isn’t their responsibility to promote options for maternity care, said Aisling Dixon, chairperson of Community Midwives Association.
“But it is a HSE service,” she said, in the same way that hospital maternity care and GP care are HSE services. They’re not being asked to promote “something that isn’t accepted”.
Dixon suggested that an information leaflet on care choices “should be given to all women on confirmation of their pregnancy”. This, as well as public awareness campaigns, was also a common suggestion from women we interviewed.
- Noteworthy, the crowdfunded community-led investigative platform from The Journal, supports independent and impactful public interest journalism. Support our work here>>
When the HSE was informed by Noteworthy about lack of choices being offered as well as pushback on birth options by some GPs, a spokesperson said that “regardless of their intended choice of pathway, all women are advised to register with their GP and to book with the maternity hospital of their choice”.
No response was provided to us by the HSE on training for GPs or provision of information to women. A HSE booklet available online – My Pregnancy – does detail the different antenatal care available during pregnancy.
We also put questions to an Irish College of General Practitioners (ICGP) representative but were directed to the HSE in relation to these queries.
Public or private?
This is an extremely loaded question when it comes to maternity care in Ireland, with many not realising the implications of each choice.
When public, semi-private and private options are presented by GPs, women told us prior knowledge was often assumed and few explanations were offered.
Private is obstetrician-led, with midwifery support. Women usually choose this option in order to have continuity of care under a consultant and the possibility of a private hospital room. It has become less popular in Ireland over the past decade.
However, choosing private can limit your choice of maternity care and exclude you from services such as community midwifery clinics or early transfer home.
For those who go public, three pathways of care await, classed by pregnancy risk level – Supported, Assisted and Specialist.
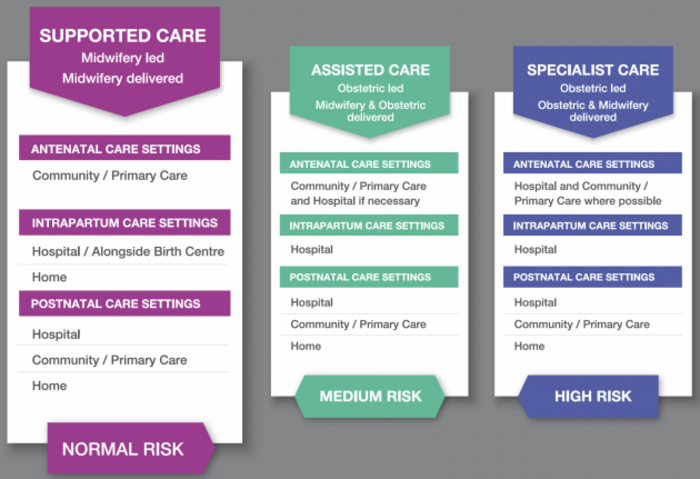 Three pathways of care exist in the public maternity system
Three pathways of care exist in the public maternity system
The ‘Supported Care‘ pathway is for healthy women with uncomplicated, normal-risk pregnancies. The HSE told us that 25-30% of women follow this path.
This is significantly lower than the potential number of women classed as ‘normal risk’, estimated to be roughly 60% in Ireland.
As part of this pathway, community care is provided to women who fall within catchment areas of certain maternity units. This includes the Domino scheme where women usually go to a community clinic during pregnancy and give birth in hospital.
In the UK, low-risk women can give birth in four places – at home, in a midwife-led unit alongside a maternity unit or standalone, or in an obstetric labour ward.
Low-risk women there are also told that giving birth in a midwifery-led unit “is particularly suitable for them” because of lower rates of interventions and similar outcomes for babies compared with obstetric units.
Ireland, unlike the UK, does not have any standalone midwifery-led units or birthing centres. These were not recommended in our Maternity Strategy.
Dr Peter Boylan, retired obstetrician and former master of the National Maternity Hospital, strongly opposes “isolated midwifery-led units”, as well as the terms ‘midwife-led’ and ‘doctor-led’. “Units should be run together with cooperation,” he says.
He told Noteworthy that “it’s important to understand that the ultimate responsibility for the outcome will probably rest with the doctor”.
Historically, that was true, but there are more midwives in court now, according to Lynda Moore, staff midwife and Irish Nurses and Midwives Organisation (INMO) representative.
“Midwifery-led care is a way of making women safer in childbirth,” she added.
- Noteworthy, the crowdfunded community-led investigative platform from The Journal, supports independent and impactful public interest journalism.Support our work here>>
International evidence has consistently shown a reduction in interventions in women who opt for midwifery-led care, according to Professor Richard Greene, director of the National Perinatal Epidemiology Centre (NPEC) and professor of obstetrics at UCC.
What is not so clear is why this is the case, he added. Some research does highlight the benefit of the relationship between the midwife and woman.
“It’s probably the fact that they’re seeing the same healthcare professional on a regular basis.” This gives time to discuss concerns, fears and anxieties, enabling women to be more psychologically prepared for labour, Greene said.
“That’s something that we can bring to all our care pathways. We probably need to be moving towards giving women a little bit more time.”
Ireland has just two ‘alongside’ midwifery-led units (MLUs) in Cavan General Hospital and Our Lady of Lourdes Hospital, Drogheda.
In these units, women are seen at every stage of their journey from pregnancy to birth to postnatal care, leading to increased consistency in care. A key difference is that midwives, rather than obstetricians, are responsible for women’s care.
Fiona Molony, manager of Drogheda’s MLU: What is a midwifery-led unit?
‘Unmet demand’ for home births
Home births are also an option but only in certain counties and for those who fit the HSE’s strict criteria. For these, many antenatal and postnatal visits are also done in the home.
Less than 1% of women avail of this service, though numbers have almost doubled in recent years, likely due to Covid maternity restrictions.
Midwives told us that women are being turned away from the HSE Home Birth Service. There is “absolutely an unmet need”, said Dixon, with just 23 self-employed community midwives operating the service across the country.
The HSE was to assess the level of demand for home births by the end of last year. This was a key action of the National Maternity Strategy. It was also to establish a stakeholder engagement process “to inform the provision” of this service.
Noteworthy asked for copies of reports, assessments, plans and submissions in relation to these actions through a Freedom of Information request (FOI) request.
It appears these weren’t complete or there was little associated paperwork, as “no records exist”, according to the HSE’s FOI response.
When this was queried, a HSE spokesperson said that it “has, and will continue to, engage with relevant stakeholders” to inform the provision of home birth services.
A number of women told us they arranged a private home birth due to lack of service by the HSE in their area. Packages from Private Midwives Ireland, the company that provides this service here, vary from around €5,000 to over €9,000.
All women we interviewed who had registered for a home birth spoke extremely highly of the continuity of care as one community midwife is present throughout.
Yvonne on choosing a home birth: ‘Why would I do it any other way?’
Maternity services ‘highly medicalised’
The care of women with medium- or high-risk pregnancies is led by an obstetrician and births take place in a hospital. ‘Assisted Care’ is for medium-risk and can involve a mix of community care by midwives and hospital care.
The most medicalised option, ‘Specialist Care’, is for high-risk pregnancies and entirely hospital-centric. It continues to be the only option available for women in certain areas of Ireland, no matter what their risk profile is.
“Maternity services in Ireland are highly medicalised – highly obstetric-led and hospital focused,” Dixon said. “We are well behind what’s considered to be an acceptable standard of choice in maternity care.”
However, when it comes to results in the current system, Boylan said that they are “fantastic now”. And though there continue to be tragedies, he said “very few babies die during labour” and “very few mothers die”.
Ireland’s perinatal mortality – which includes stillbirths and deaths of very young babies – decreased by over a percentage point in the past decade. Research showed this decrease occurred across all groups except African born mothers, where the rate increased.
Inequalities in maternity outcomes are well documented, with guidelines from the National Institute for Health and Care Excellence (NICE) in the UK outlining that compared to white babies, the stillbirth rate is twice as high in black babies and 50% higher in Asian babies.
It recommends that women from some minority ethnic backgrounds or who live in deprived areas “may benefit from closer monitoring and additional support”.
Black women are also almost two times more likely to die than white women. Asian women are almost twice as likely to die.
A number of maternal deaths do occur in Ireland every year, with some – including any related to less familiar options such as home births – receiving significantly more news coverage than others.
The highest in recent years was when six women died in 2018. Deaths which occur during pregnancy, labour and birth as well as over a month after having a baby are classed as maternal deaths.
In contrast to Ireland, latest analysis shows that there has been a “statistically significant increase in maternal death rate in the UK” from causes directly related to pregnancy.
Women’s choice ‘not always supported’
By opting private or semi-private, women in most areas are automatically funnelling themselves into services akin to the ‘Specialised Care’ pathway.
This is a problem, according to Sunita Panda, midwife and researcher from Trinity College Dublin (TCD). She has extensively researched caesarean sections in first-time mothers, examining the hospital records of over 2,700 women.
“A lot of low-risk women go for private care” when they could be availing of midwifery services, according to Panda. Her research, alongside many other studies, has found that more planned and unplanned caesarean sections occur in private care.
Research from 2020 found that first-time mothers attending an obstetrician privately are more than twice as likely to have a caesarean birth, despite not having a higher at-risk profile.
Panda conducted in-depth interviews with obstetricians for her research. She told Noteworthy that none mentioned encouraging a low- or normal-risk woman to instead avail of public midwifery antenatal services, even though this option is encouraged for women in this risk profile outside of private care.
A different solution for lower-risk women is proposed by Boylan – private care that shares care with public community midwives, in the same way that shared care occurs now between hospitals and GPs.
That’s just a matter for doctors and midwives to sit down together and work out.
Though many obstetricians support midwifery-led care in Ireland, pushback has been documented at certain maternity units and almost led to the closure of the midwifery-led unit (MLU) in Cavan.
Following public outrage over the planned closure, a report in 2020 found two major challenges were caused by doctors. We obtained this report through FOI and have made it available online here.
GPs weren’t referring patients to the MLU, with women’s choice “not always supported”.
And almost all women (94.5%) referred to obstetricians for scans, growth queries and other reasons were not transferred back to the MLU’s care.
The report did not examine adverse clinical outcomes given “no evidence” of this being an issue, yet the unit had been set to close. It didn’t in the end, following protests. A number of actions, including easier GP referral and more discussions between obstetricians and midwives, were recommended.
SECOND TRIMESTER: Being ‘a difficult patient’

You’ve made your choice. The challenge now is being allowed to stick with it.
Cork woman Niamh McAleer wanted to have a home birth for her second pregnancy after feeling like she hadn’t been given a choice over some of the medical interventions she received during her first.
This included a membrane sweep around the neck of her womb which, she said, was done during a vaginal exam without her consent.
She was initially accepted onto the home birth scheme but became ineligible after a test showed her baby was at 2% risk of anaemia.
So ensued her first fight, to be transferred onto the Domino scheme – the mix of community midwifery and hospital care.
She had to fight again when it came to planning the hospital birth. She wanted to use the pool during labour but was told she couldn’t unless she agreed to a period of continuous electronic fetal monitoring – something she felt was unnecessary.
Irish national guidelines state that “the quality of the evidence that underpins much of the practice in fetal heart rate monitoring is moderate at best”. Instead, they recommend intermediate monitoring as standard, unless there are specific risks, none of which McAleer had.
I was made feel like I was a ‘difficult patient’ and told I couldn’t avail of [the] pool due to my decision.
It took escalating it to the director of nursing as well as a patient advocacy officer before she was told – a week before her due date – that she was low-risk and could use the pool.
“Fighting the system,” she said, for the last few weeks of her pregnancy “caused so much stress”.
McAleer is not unique. Inconsistent policies in different maternity units frustrated a number of women and limited their care choices.
We asked the HSE if it had any plans to standardise maternity care across all hospital groups. A spokesperson said that the role of the National Women and Infants Health Programme (NWIHP) “is to lead on the management, organisation and delivery of maternity, gynaecology and neonatal services”.
“A key focus for NWIHP is the standardisation of clinical pathways and clinical practice guidelines. The NWIHP acknowledges that there is evidence of some variation between units and will continue to work to reduce/minimise same.”
Discharged from GP care
GP cover for women choosing to have home births is another inconsistent aspect of maternity care.
When Erin Devitt’s GP found out she was planning a home birth through the HSE scheme, she was discharged at 28 weeks pregnant. This was because her GP’s medical indemnity insurance did not cover her to treat women planning to give birth at home.
She wasn’t accepted back until her baby was two weeks old, leaving her without GP support and feeling like she was doing something outside the system.
You shouldn’t be made feel that you’re doing something dangerous.
This is a common problem for those planning home births as only certain medical indemnity providers provide cover to GPs.
“As GPs are private practitioners”, they are required to “arrange professional indemnity cover from private medical indemnity providers”, according to a spokesperson for the Department of Health. They added that “such arrangements are a matter between the two private parties concerned”.
In May, the HSE said it was examining the role of GPs as part of a review of the wider Maternity and Infant Care Scheme.
When we queried what it was doing to address issues with insurance cover, a HSE spokesperson said that “further discussions need to take place with relevant parties, including indemnifying organisations, to agree national policy on the role of the GPs in relation to home births”.
Over 4,000 people signed a petition on this issue a few years ago and it was also the subject of a Workplace Relations Commission case in 2019 against provider Medisec Ireland.
Noteworthy put this issue to three of the main providers. No response was received from Medisec Ireland or Challenge.
Dr Sarah Townley, Deputy Medical Director at Medical Protection said that GPs are covered for “medicolegal issues arising from the antenatal care of patients registered with the HSE home birth scheme” as well as for certain routine baby and maternal checks.
Because of these obstacles as well as pushback by healthcare professionals at all levels, many women told us that they hid the fact that they were planning a home birth at GP appointments and hospital clinics until a few weeks before their due date.
When asked for his views on home births, Boylan said that “on a first birth” he would be “a little bit wary”. He said a “good compromise” would be care by a midwife at home with a hospital birth, but a quick discharge.
“If all has gone well on a first birth, then it’s very unlikely that there’d be a problem on a second birth. In those circumstances, a home birth is probably a very reasonable thing.”
UK Research of over 64,000 low-risk births – used in NICE guidelines – found that, for women who had already given birth, home births resulted in lower rates of interventions and outcomes for babies that were no different.
Home births have faced many restrictions in recent years, most notably a continued suspension by University Maternity Hospital Limerick after the death of Laura Liston following a transfer from home to hospital last year.
A potential 30-minute ‘blue light’ limit could also prevent women in large parts of rural Ireland from accessing the service. We reported yesterday that this controversial guidance “remains in place”, according to the HSE.
We also investigated water births and found the tide is gradually turning, with Drogheda becoming the third hospital to reinstate this option.
Lack of middle-ground options
Home births do not suit everyone, but few middle-ground options exist between home births and highly medicalised hospital births in parts of Ireland, community midwife Dixon pointed out.
This middle-ground of midwifery was to be addressed by the National Maternity Strategy through the supported care pathway. However, a 2020 Health Information and Quality Authority (HIQA) report found that the pathway’s progress “was relatively limited, and generally predated” the strategy.
“There’s a bit more work being done for midwives to undertake that care,” according to obstetrician Prof Richard Greene. Though he acknowledged that “it hasn’t happened as quickly as it should have happened.”
Cork University Maternity Hospital has “done a whole piece of work” to ensure that “when women are seen for their booking visit” are offered supported care if they fit that category. He said that a number of other maternity units are working on improving this.
Though progress has since been made in some areas, Noteworthy investigated the recommendation that women “in the Supported Care pathway will give birth in an Alongside Birth Centre”.
The midwifery-led units (MLUs) in Cavan and Drogheda are the only Irish ‘alongside birth centres’, per the standard classification. That is relevant as in its implementation of the Maternity Strategy, the HSE has muddied – and confused – the waters somewhat, allowing it to claim progress that many feel it hasn’t actually made.
We requested plans to address the development of these, a key action in the Strategy’s Implementation Plan which was due at the end of last year. The HSE said that “no records existed” in response to our FOI.
When this was queried, a HSE spokesperson said that “infrastructure challenges” are present on many of the existing clinical sites so the focus of the NWIHP “is currently on the development of home-away-from-home delivery suites within the maternity services”.
As of now, 15 of the 19 maternity units now have such suites in place.
“These suites effectively replicate the environment and birthing infrastructure available” in the MLUs, a HSE spokesperson told Noteworthy. “There is dedicated clinical space, including two specifically-designed delivery suites to enable and support midwifery-provided maternity services to women in their region.”
However, these operate differently to alongside birthing units, according to midwives who spoke to Noteworthy. Though the surroundings are improved, the provision of care is usually still obstetric rather than midwife-led.
For instance, in Cork University Maternity Hospital, there is no alongside unit and their home-away-from-home rooms aren’t “used only for midwifery care”, according to staff midwife and INMO rep Lynda Moore.
On the development of alongside birthing units, the HSE said that it and the NWIHP “remain committed to the National Maternity Strategy and will continue to work closely with all 19 maternity services so as to drive the Model of Care as recommended”.
“The development of a capital plan to address all infrastructure issues is much bigger than just maternity and needs to align to the Development Control Plan for each hospital site.”
Noteworthy requested an interview with both the National Lead Midwife Angela Dunne and the National Clinical Director Dr Cliona Murphy of the National Women and Infants Health Programme (NWIHP), but this was not accommodated by the HSE.
THIRD TRIMESTER: ‘A lot of pressure’

When choice isn’t supported, research has shown that trauma can result.
A traumatic experience during their first hospital birth led most women we interviewed to research other options of care for subsequent pregnancies.
Jodi who lives in Co Kildare was one such woman who opted for a home birth following what she called a “very traumatic birth” in hospital.
Her birth preferences stated that she wanted an intervention-free labour, if at all possible, and she was “ready to advocate” for this. This was “quite difficult” when being asked to consent to interventions between contractions.
She was given syntocinon, a drug used to stimulate contractions – something she felt wasn’t necessary on reflection as “there was no risk at that point”.
“I did sign a form which I barely remember… There was definitely no mention of the risks associated.”
Jodi on consent between contractions: ‘This is what is going to happen’
Being induced “really changed the course” of her labour and “there was a lot of pressure to get the baby born”. She then was given an episiotomy – a cut of the vaginal opening.
After that experience, Jodi opted to have her second daughter in June with a home birth which required no medical interventions. “It was completely night and day.”
Mairéad Cronin also felt her birth preferences for minimal interventions, including declining continuous electronic fetal monitoring, were not listened to.
At one point, after questioning her preferences, Cronin said a midwife went over to her medical file, “opened it, rolled her eyes and sniggered”.
She felt “unheard, belittled and made feel small”, with her energy being diverted away from the most important “task at hand”.
“A woman can only have her first baby once,” said Boylan. “It’s a unique experience and can never be repeated.
“You’ve got to concentrate on first birth… That needs to be emphasised more in teaching both for midwives and for doctors.”
Sarah Culleton on subsequent pregnancies:‘I always felt more heard”
Interventions without ‘valid clinical reason’
Like Jodi, half of the women we interviewed felt pressured into inductions or other interventions, with what they felt was no clinical indication.
Some said they were threatened or coerced.
This echoes research by TCD’s Soma Gregory who studies perceptions of care in people with experiences of both hospital and home birth. She found overwhelmingly more positive feedback was given for home births compared to hospital births.
When just looking at hospital births, “there was a cohort of respondents who had traumatic experiences,” said Gregory. This included “procedures or interventions being carried out without explicit consent”.
Even people who had good experiences, felt that “they weren’t involved” and, instead, things were happening to them.
Similarly, during TCD’s Sunita Panda’s research interviews, “many women did not know why they were being induced or if they were being induced for the right reason”.
Obstetrician Greene said that being “upfront and honest”, he would have dealt with complaints along those lines.
I’ve absolutely come across women who felt that they weren’t given appropriate information or felt that they were forced into certain situations.
This can either occur “because it happens” or because people may not hear what the medical teams are saying “in the throes of labour”. In either case, the woman had a certain experience.
Like Boylan, Greene said education was key – both of women about their options – but also of clinicians so that they take better care to prevent such situations arising. It is also important to debrief and spend time with women before discharge, in particular when something unexpected happens, he added.
Panda said that a lot of inductions “don’t actually have a valid clinical reason”. Her study across three maternity hospitals found that they increased the risk of first time mothers having a caesarean birth.
In addition, “most of the consultants, registrars and midwives strongly felt that they had a lot of unnecessary caesarean births because of failed inductions.”
Increasing caesarean sections rates are examined later this week for this series.
For induction it’s often “about convenience and control”, said staff midwife Moore. However, she said that there “is an element of consent that is done”, it is “recognised by all of us that it’s totally necessary”.
Some risks do increase when a pregnancy continues beyond 41 weeks, according to NICE guidelines on induction of labour. These include an increased likelihood of caesarean birth and the baby needing admission to a neonatal intensive care unit (NICU).
Rates of stillbirth and neonatal death also increase, with about 31 more babies expected to die per 10,000 whose mothers gave birth at 42 weeks, compared to at 41 weeks.
A HSE spokesperson said that “an important workstream of the NWIHP in conjunction with the Institute of Obstetricians and Gynaecologists of the Royal College of Physicians Ireland is the revision and update of the National Clinical Guidelines for Maternity and Gynaecology”.
A new National Clinical Practice Guideline for Induction of Labour is due to be published towards the end of this year, they added.
The Guideline will incorporate key recommendations on areas such as: indications for induction, induction methods, communication, consent and informed decision making.
For Hayley Purtill-Quin “everything changed” once she got close to being due, with frequent talk of induction by her maternity team.
“Once I got to my due date, it was awful. I spent the next 10 days worrying about being taken in for induction. It was a huge stress.”
Purtill-Quin went into labour when she was 10 days overdue and found out she was booked in for an induction, without her knowledge or permission, for the following day.
“Doulas see a lot of coercion,” said Anita Petry, chairperson of the Doula Association of Ireland. “We witness people being asked the same thing ten times when they’ve already said no.”
It’s also extremely difficult to say no to a doctor in vulnerable situations, such as during labour, she added.
Anita Petry, Doula Association of Ireland: What is a doula?
Dreaming of choice across the country
It is clear from this investigation that large gaps in choices of care, such as home births or midwifery-led services, remain for many women across Ireland.
“If the only choice available to you” is at odds with your values for your life, then “it’s going to be really hard for you to have a positive experience”, said TCD’s Gregory.
Not all clinicians we spoke to were happy with the National Maternity Strategy, but the increased focus on both community and hospital midwifery care was welcomed by most.
Key to its implementation is funding and staffing.
Just under €16m of development funding was awarded over the past three years. This included funding for “enhanced midwifery care across the three pathways”.
“Staff shortages are probably the biggest challenge” for maternity services, according to Boylan, with many others saying similar.
Both staff midwives and public health nurse numbers have decreased year-on-year. The home birth service is also stagnated due to lack of availability of the 23 self-employed community midwives.
A HSE spokesperson referenced an estimated global “shortfall of six million nurses and midwives”, with 8% more graduates needed year-on-year up to 2023. They added:
“A National Midwifery Taskforce is in the process of being established to identify and address issues relating to supply and demand, retention, and recruitment of nursing and midwifery staff.”
In addition to the traditional college route, INMO official Bernadette Stenson said the sponsorship model should be expanded. This is where staff, such as healthcare assistants, retain their basic salary while training to become nurses or midwives.
She added that numbers being recruited after training “is a significant issue” and needed to increase.
Out of all the women we spoke to, Sarah Culleton from Co Waterford had a clear vision for Irish maternity care. She felt “unheard” while giving birth to her second son near the start of the pandemic and subsequently availed of the Domino community scheme and a home birth.
And what is Culleton’s dream?
“If I was ever to win the lotto I would love to set up a load of midwife-led units around Ireland.”
Not the usual lotto spend but a reflection on the desire for choice by many here.
—
Read more articles in this series >>

Why does the Irish health service offer so little choice for expectant mothers?

By Maria Delaney of Noteworthy
Noteworthy is the crowdfunded investigative journalism platform from The Journal. This investigation was proposed and funded by our readers alongside direct support from our investigative fund.
What’s next? We also want to uncover how a broken system is detrimentally impacting women’s health. Help fund this work >>






