'I am struggling': How home carers became the forgotten frontline workers of the pandemic
Part one of Noteworthy’s in-depth investigation shows that many carers took a pay hit and felt unsupported during the Covid-19 crisis.

“WE DON’T KNOW from month to month if we are going to get paid for [cancelled] hours.”
Ellen McNamee is a home carer in the not-for-profit sector who works with both older people and people with disabilities. The worry over getting paid for clients who cancelled their care has affected her and her colleagues over the past few months, with many experiencing a significant drop in their paycheck.
“We have had to wait for a letter or text message from our job.” Even this month, with two clients cancelled, McNamee doesn’t know if she will be compensated for these lost hours.
This is due to the nature of their contracts, she explained, as hours are not guaranteed from week to week. As a SIPTU shop steward, she speaks regularly to other carers in the sector.
“I had girls crying. We still have bills and mortgages to pay. It was worrying. Carers in the community were keeping clients out of hospital but we were forgotten about.”
 Ellen McNamee says uncertainty over pay has been a worry for home carers during the pandemic
Ellen McNamee says uncertainty over pay has been a worry for home carers during the pandemic
Over the past number of weeks, Noteworthy has taken a deep dive into the home care sector. In the first of our three-part investigation, we show that many carers took a pay hit and felt unsupported by their companies during the pandemic. We reveal:
- Carers experienced significant income loss due to Covid-19 in spite of the HSE agreeing to pay providers for the months when the pandemic peaked.
- There were significant issues with access to enhanced personal protective equipment (PPE) in the sector, with some carers not receiving face masks until May – and some being told by employers to buy masks themselves.
- Some reports of lack of support for those caring for clients with suspected or confirmed Covid-19. A number of carers told Noteworthy that they were not advised that their client was suspected to have the virus, meaning some became close contacts without being given the option of taking this risk.
- An estimated half of undocumented live-in carers, employed by private families, worked more hours with no extra pay, with some reporting no breaks or days off for the duration of the lockdown.
- Family carers continue to worry about the restoration of home care and other health services.
In part two of the investigation, we examine the pay and conditions of these vital frontline workers, as well as the profits made by providers. Finally, in part three, we will reveal the impact that lack of regulation is having on home care and assess the future of the sector.
Loss of pay in spite of public funding to providers
Unlike in nursing homes, the home care sector did not have a crisis in terms of virus spread, but a major problem that impacted the entire sector was the loss of clients who were advised to cocoon.
Some carers told Noteworthy that they experienced significant income loss due to Covid-19 either due to cancelled hours or having to self isolate after being a close contact of a client who tested positive. This is in spite of the HSE agreeing to pay providers who had to isolate as a result of their work.
Cancellation of clients had a huge impact on providers, according to Joseph Musgrave, chief executive of the representative body for private for-profit providers, Home and Community Care Ireland (HCCI). HCCI represents around 80 providers in Ireland who care for 20,000 people and employ 10,000 carers.
We had 4,000 clients suspend their care on the week of 12 April. That’s huge and impacts every element of our service.
This was made more problematic due to the current home care structure, explained Musgrave. “The way carers are paid and the way the HSE pays providers is for every hour of care delivered. So if you’re not delivering an hour of care, then you don’t get paid.”
A spokesperson for the HSE said it “engaged extensively” with both HCCI and NCCN – the National Community Care Network who represent voluntary not-for-profit providers – throughout the pandemic.
It initially “agreed to pay providers an agreed rate in respect of clients who were cancelling their service from 13 March”. During this time, providers were only paid for the first two days when a client self-isolated.
Subsequently this policy was revised from the start of April and providers were “paid at 01 March levels of service to end May 2020”. Payments reverted to “normal service arrangements” from the start of June.
However, these payments were not always passed on to carers, though it appears that most providers did pass on as much pay as they could to their staff. Musgrave said that with so many clients suddenly cancelling in March, providers may have thought that if they passed on cancellation payments to staff, they may not have been able to stay in business by the end of the month.
“Providers were saying: ‘I’m losing far more money than the HSE is paying me and I’ve got all my overheads, staff still on the books’,” he added. Though it appears that most providers did pass on as much pay as they could to carers.
Because of this, “some providers paid their carers in March and took the hit but some couldn’t do that”.
Musgrave explained a different system was implemented in April which meant that the HSE would “pay the average of what you were being paid before the pandemic and that means you would continue to pay your carers”.
Providers were also unable to plan ahead as the new policy in April was initially only for a short period and then it was renewed, explained Musgrave. “It was very confusing and complicated.”
In terms of the April and May payment, Musgrave said that his “understanding is that most HCCI members did pass on as much pay as they could to carers” but he added that he couldn’t speak for non-HCCI members.
We asked the top five HSE funded for-profit private home care providers if they passed on these HSE payments to their carers if their hours were cut. These five companies are all members of HCCI. Here are their responses:
This table can also be viewed here.
A number of carers from Home Instead Senior Care told Noteworthy that they experienced income loss over the course of the pandemic. This for-profit provider received the most HSE funding over the past number of years, with €55.5 million paid to them in 2019.
“All Home Instead CAREGivers are paid for the work they do,” according to the provider, who also stated: “As you can appreciate, the home care sector has experienced challenges over the last number of months and we have worked closely with the HSE to continue to provide care for vulnerable seniors in our community.”
Emily*, a carer for Home Instead in the West of Ireland, said that because one of her clients had suspected Covid-19, her work was limited to that one client for over two weeks while awaiting the test results. Her income dropped significantly to €80 per week because of this.
“I wasn’t entitled to any Covid payment,” she said, and has not, as yet, received any compensation for those lost hours. The test subsequently came back negative so she could return to her other clients.

However, other carers were treated differently. Megan*, a home carer based in Dublin who works for a Dublin branch of the same private provider, said that she was paid her normal wage when looking after a client who had coronavirus, even though her hours were cut as she couldn’t look after her other clients.
In a statement to Noteworthy, Home Instead said:
“As part of the national response to Covid-19, the HSE put a nationwide agreement in place with homecare providers to deal with the challenges posed by the pandemic. This included provision of care not previously anticipated, cancellations, redeployment or alterations to scheduled care, and other responsive requirements. While this had some operational and income impacts both on our overall business and CAREGivers, these impacts were minimised.”
Carers told to ‘buy face masks’
Healthcare workers made up over 30% of reported cases of Covid-19 in Ireland, which equates to over 8,400 cases to date. There were over 2,200 cases reported in healthcare assistants (HCAs) in all settings.
The Health Protection Surveillance Centre (HPSC) told Noteworthy that, as of 18 July, “51 cases were reported as working as home care workers”. It also reported “there have been no Covid-19 notified deaths in home care workers”.
It listed the number of outbreaks, clusters and associated deaths within the home care sector:
The HPSC has advised that ten Covid-19 clusters have been notified which were associated with home care workers and/or their clients (2,282 outbreaks in total have been notified). A total of 52 Covid-19 cases are linked to these outbreaks. Of the 52 cases, 17 were reported as healthcare workers. There have been a total of six notified deaths associated with these clusters.
In comparison, there were almost 270 clusters associated with nursing homes and over 170 at residential institutions during the same time period.
Toward the start of the pandemic, when Emily was caring for a client with suspected coronavirus, she wasn’t supplied with any extra PPE. This was true for a number of carers who contacted Noteworthy.
When they were informed of this by Noteworthy, a spokesperson for the provider said: “From the outset of the pandemic, Home Instead Senior Care has adhered in full to the HSE, NPHET and HPSC guidelines”.
The HPSC did not advise home carers to wear masks unless their client had confirmed Covid-19 before new guidance was issued on 22 April. Between 17 March and that date, its guidance stated:
This guidance DOES NOT RECOMMEND use of surgical face masks in situations other than for contact with patients with droplet transmitted infection including COVID-19.
The care workers that Noteworthy spoke to were all given plastic aprons and gloves prior to the pandemic and this continued to be the only PPE for many when Covid-19 cases were increasing in Ireland at the end of March and during April. Most said when they asked about this, their employer cited HSE guidance which had not recommended masks at the time.
Some were told by their employers that they could “buy face masks themselves”, without offering a reimbursement, but carers said this was not plausible due to both supply and cost.
In April, HCA and Carers Ireland found that 44% of carers and healthcare assistants they surveyed only had access to either an apron, gloves or both, with 3% having no PPE at all. At that time just over half of carers were using face masks.
This issue was not unique to the private sector and it also impacted the HSE and nonprofits. In the early days of the pandemic, HSE workers had to buy their own masks and gloves, according to Marie Butler, healthcare assistants’ sector organiser for SIPTU, though this issue seems to have now leveled out somewhat, she added.
On the recommendation of the National Public Health Emergency Team (NPHET), the HPSC issued new guidance on 22 April on the use of surgical masks in healthcare settings which included recommendations for home carers to wear face masks to protect against Covid-19.
HCCI’s Musgrave was concerned about where the private sector was going to source face masks. He said:
Ten days went by [after the guidance was issued] and we heard nothing, despite many calls and emails about what was going to happen.
“Eventually, after some debate, the HSE decided they were going to supply the entire sector with face masks,” he added.
Since these were not included in the service agreements for HSE contracts, the HSE subsequently agreed to provide “enhanced PPE” which included face masks to private and nonprofit providers. The HSE told Noteworthy that “every effort is made to ensure appropriate PPE is available to ensure continued provision of home support service, especially to those clients with higher priority needs”.
Noteworthy has seen emails from one large home care provider showing that it wasn’t until mid-May that the masks arrived in their office and could be distributed to carers, meaning that many home carers worked through the peak of the pandemic in Ireland without them.
Though there were a number of problems initially with access to enhanced PPE for suspected and confirmed cases, this “stabilised relatively quickly without too many problems” towards the end of April due to the low amount of the virus in the sector, recalled Musgrave. “If that had spiked, it would have been a huge issue, but thankfully it didn’t.”
HCA and Carers Ireland conducted a private survey recently, after the pandemic had peaked. With over 1,100 respondents, they found that in the private sector the majority of carers are now getting access to sufficient PPE.
Public health and HSE advice was followed at all times, according to a spokesperson from Comfort Keepers. They added that their “carers have been equipped with the correct levels of PPE to do their job at all times”.
Comfort Keepers have always provided PPE to our staff and when advanced PPE was advised by Public Health which included masks, masks were provided to all staff.
“PPE was provided at no cost to our staff in order to help keep not only them safe, but our customers safe too,” according to Bluebird Care UK, which took over the Irish franchise in June. A spokesperson said it was “a little tricky to comment” on earlier months but added the approaches taken by the UK company, were “often replicated” in Ireland.
Caremark Ireland said that “masks are provided to all staff at no cost since public health guidance was issued [regarding] same”. Home Instead, Irish Homecare and Comfort Keepers also said they provide PPE to their staff at no cost.
Regarding the provision of face masks, John Florence, chief executive of Irish Homecare, said they “followed public health advice at all times and masks were made available to all staff from March”. He added:
Where carers had bought masks themselves, we provided full reimbursement, so that none of them were out of pocket. We continue to take this approach today.
Training during Covid-19 was also mentioned by the providers we contacted. Bluebird Care “invested heavily in protecting both our staff and customers and also in additional training” and Comfort Keepers “provided new Covid-19 infection control training, extra refresher training and online courses to ensure PPE was being used correctly”.
‘Selfcare is not allowed’
Mental health has been raised as an issue across all sections of society during the pandemic, with issues such as lack of PPE adding to this.
Suspected and positive cases of Covid-19 were particularly stressful experiences for home carers that contacted Noteworthy. A number of carers recounted experiences of not knowing their client had suspected or confirmed coronavirus.

Her client was hospitalised and diagnosed with Covid-19. Since she was in such close contact, Noreen had to isolate and missed work for two weeks. She later tested negative for the virus.
“The HSE provided mental health support that was open to all healthcare workers,” said Metcalfe of HCA and Carers Ireland, but added it is unclear what assistance was provided by private companies.
“In terms of the mental health of our carers, we are very aware of the impact that the pandemic has on people,” said Florence of Irish Homecare. He added:
We made contact with every single one of our carers and asked them if they were happy to work through the pandemic. Most of our carers have now returned to work and are happy with the supports we have provided.
A welfare and wellness programme was implemented by Comfort Keepers “which included daily and weekly welfare check-ins” as well as other supports such as a hardship fund and access to an employee assistance programme. “Support, guidance and training” was provided to all caregivers, according to a spokesperson for Home Instead.
“We take the wellbeing and mental health of all our staff seriously,” said Caremark who said support is available 24/7. Bluebird Care in the UK, which now owns the Irish franchise, told Noteworthy that from a network-wide survey it conducted their “businesses were supporting their teams exceptionally well, despite the circumstances”.
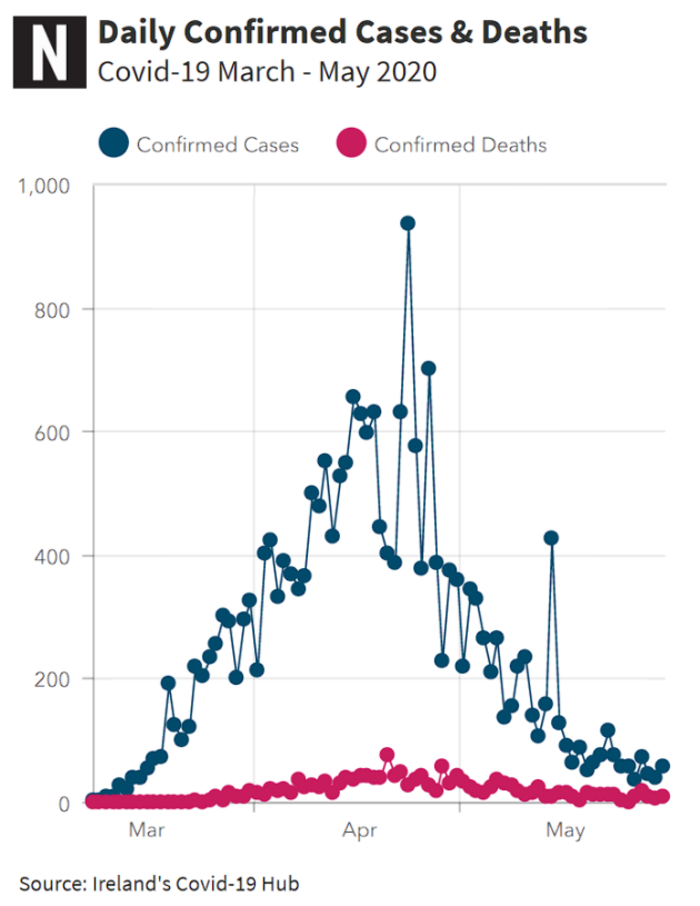
An interactive version of this graph can be found here.
HCAs and carers were already stressed before the pandemic, according to a joint study released by HCA and Carers Ireland as well as UCD earlier this year. It found that 31% of those working in home care reported significant stress or distress. Private sector home carers had a marginally higher level of distress.
“Selfcare is not allowed within many private sector settings,” the study found. Carers struggle after the death of a client as well as due to workload. This results in carers being “at risk of recurrent burnout”, with many “becoming addicted to nicotine, caffeine and negative health risks”.
‘Afraid to voice what we want’
One group of private carers whose conditions worsened during the pandemic were live-in carers, many of whom are undocumented migrant workers in Ireland.
A recent survey by the Migrant Rights Centre Ireland (MRCI) found that almost 60% of respondents, who were mainly employed by private families, were working more hours since the Covid-19 crisis hit but over 50% were not getting paid for extra hours.
Over 30% of the carers were working seven days a week and the average working time reported was 77 hours, well above the maximum average working of 48 hours.
Ten carers surveyed reported working 24/7 and Linda Keitasha, care community development officer at MRCI, said that this is because they were on duty with no relief from other carers or family members who would usually help out. “These women, 12 weeks in, were not getting a day off and weren’t getting paid extra,” she explained.
An interactive version of this graph can be found here.
Getting paid between €400 and €550 per week with such high working hours “with no real working conditions, entitlements or clear breaks”, means that many of these carers are working for multiples below the minimum wage, according to Keitasha.
One undocumented carer in this position was Gwen* who is from the Philippines and has been working in Ireland for a number of years to support her family at home. She had no breaks over a 15-week period during the pandemic and was on duty 24/7.
“It’s really hard especially when we are the only two here all night and day.” Gwen normally had the weekend off but the family member who normally helped out worked on the frontline so could not care for their older relative. “I understand as their [relative] has an underlying illness,” she explained.
“They only paid me for the week days and not the [extra] two days,” she explained. “They promised me that after Covid, they will give me a holiday for a week.” She isn’t sure if she will get paid for this break yet either.
Undocumented workers find it difficult to raise issues of pay and conditions with their employers, according to Keitasha. She explained “it’s an area where huge exploitation occurs”, adding there is often a power imbalance between live-in carers as they can fear being reported or sent home.
Gwen said she is “ashamed to say they should pay me for the two [extra] days [per week] because they’re very good so I don’t want to complain about my salary”.

She hopes that the new Government will hear their voice and “give us a permanent regularisation so we can live here”.
This is what the MRCI wants for the estimated 20,000 undocumented migrants in Ireland, said Keitasha. The pandemic highlighted how important “essential workers are but after Covid is long gone, they will be forgotten about”.
The Programme for Government committed to “create new pathways for long-term undocumented people and their dependents meeting specified criteria to regularise their status within 18 months of the formation of the Government”. A spokesperson for the Department of Justice told Noteworthy that “a policy paper on the matter is being drafted by the Department at the present time”.
Family carers severely impacted
Family carers, who provide regular care to friends or family members, are another group of carers that has been severely impacted by the pandemic, according to Catherine Cox from Family Carers Ireland, an organisation who both advocates for family carers as well as a not for profit home care provider.
This was due to the withdrawal of supports such as home care, respite and day care as well as reduced support from extended family members. A survey by the organisation during the pandemic found that one in three family carers experienced a reduction or cancellation in home care services.

Aisling Harmon cares for her mother who has Parkinson’s having previously also looked after her father who died three years ago. She feels that family carers have “never been more invisible” than they are now.
Access to services that “give you that bit of light at the end of your tunnel” such as the physio or speech and language visits became unavailable. These changes have also been “frightening for those who are cared for”, Harmon added.
The HSE told Noteworthy that due to the pandemic it “had to reassess its operation of Home Support Services, to ensure that the needs of those client’s with the highest priority” were met. The HSE will continue “to restore services over the coming weeks”.

‘Home has been a safe place’
Although there were many problems in the home care sector over the past number of months in terms of protection of workers, it had a lower number of outbreaks and cases compared to nursing homes.
This was “one of the success stories of the pandemic, if you could call it that”, said Marie Butler, healthcare assistants’ sector organiser for SIPTU.
HCCI’s Musgrave said this shows that “home has been a safe place to care for people but it is still a very vulnerable population”. He said that about half of the clients that tested positive for the virus needed to be hospitalised.
“This is in stark contrast to congregated care settings where if you have a lot of vulnerable people in a small place, unfortunately it’s a difficult place to control the virus.”
***
Some of the issues explored in this article are exacerbated by a lack of regulation in the sector, according to many experts. In part three of this investigation, Noteworthy will delve into this issue by examining what’s in store for the future of the sector. But first, in part two, we examine the pay and conditions of these vital frontline workers, as well as the profits made by providers.
*Names have been changed due to requested anonymity
***

This investigation was carried out by Maria Delaney of Noteworthy. It was proposed and funded by you, our readers, as well as with support from the Noteworthy general fund.
Due to the volume of issues raised by carers about the home care sector when they answered our call-out, we decided to expand the investigation into a three-part series. If you would like to help towards the cost of this additional work, please support the general fund here.
Noteworthy is the investigative journalism platform from TheJournal.ie. You can support our work by helping to fund one of our other investigation proposals or submitting an idea for a story. Click here to find out more >>







